Hi all, Today we have a guest post from Dr. David Lendrum, an ER physician at the Foothills Hospital in Calgary. Dave is a super brilliant doc, and this post will outline how to perform BIPAP using a ventilator, as opposed to bringing an extra BIPAP machine into an already crowded resus area. This is […]
SOCMOB How To: Make Your Own End-Tidal CO2 Detector
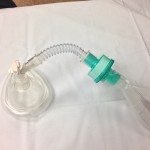
Hey SOCMOBBERS, The ASA now recommends that all procedural sedations (not conscious sedations!) be done with quantitative waveform capnography. While I understand it’s not feasible in some places, capnography is a hugely valuable tool, and detects apnea long before the pulse ox reading drops. Where I work, there are no fancy nasal prongs or face […]