Previously we have discussed the use of propofol for migraine headache (part 1, part 2). In this post, we’ll look at another headache treatment that can be added to your armamentarium, the paraspinous cervical block. There are many standard cocktails for headache management in the ED, but unfortunately, many of these require an IV, fluids, […]
SOCMOB How To: Using the Ventilator for DSI with Dave Lendrum
Hi all, Today we have a guest post from Dr. David Lendrum, an ER physician at the Foothills Hospital in Calgary. Dave is a super brilliant doc, and this post will outline how to perform BIPAP using a ventilator, as opposed to bringing an extra BIPAP machine into an already crowded resus area. This is […]
Digital Intubation, and I Don’t Mean Video
Hey all, Listening to the May edition of EM:RAP yesterday, there was a segment by Patrick Shipsey on digital intubation. At first I thought this would be the same old, same old. That is, someone discussing the pros and cons of video and direct laryngoscopy. What I didn’t expect to hear was someone talking about […]
SOCMOB How To: Jet Insufflation and Bougie Assisted Cric
Hi all, A few months back we looked at how to make your own cricothyrotomy trainer. Easy and inexpensive, you can find the video here. Today I’m adding two more procedure videos which demonstrate a simple jet insufflation setup, as well as the bougie-assisted cricothyrotomy. Shout out to Darren Braude of EM:RAP and many other […]
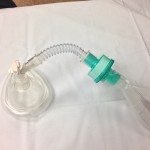
SOCMOB How To: Make an atomizer device
It’s time for another video. Today I’ll be showing you how to MacGyver your own atomizer for intranasal and orotracheal drug administration. Shout outs to fellow USask FOAMite Dr. Nadim Lalani (@ERMentor) and Dr. Whit Fisher for the idea behind this one. Today’s video is a modification of the design outlined by Whit Fisher here. […]